- Law & Policy
- Regulation & Property Rights
- Politics, Institutions, and Public Opinion
- Health Care
- Economics
The number of obese Americans has sharply increased in the past 30 years. The typical American diet—which too often counts doughnuts and french fries as staples—is not what doctors and nutritionists would like it to be. Also, many of us do not exercise frequently enough. Our gluttony and sloth lead inexorably to bulging waistlines, chronic disease, missed workdays, high health-care costs, and premature death. To many minds, these problems suggest a first-order public health crisis.
But is obesity really a public health crisis, or is it merely a private health affliction that too many of us face? The distinction is important because public health crises are often used to justify muscular government action. Banning trans fats in New York restaurants, restricting portion sizes at fast-food restaurants, and putting “sin” taxes on junk food are easier to ratio-nalize if there is a public crisis.
What distinguishes a public health crisis from a large-scale private health crisis? The public health literature offers—no surprise—an expansive definition of a public health crisis. In that literature, a public health crisis arises whenever any undesirable health state becomes sufficiently widespread. By this standard, all private health issues are public, and the personal is by definition political.
The problem with this approach is that it collapses a vital distinction between diseases and health conditions that harm the health and well-being of others, and conditions that adversely affect only those with the condition. A sharp increase in the prevalence of a dangerous infectious disease like tuberculosis is no doubt a public health emergency, but the same is not true for an increase in back pain. In the case of tuberculosis, drastic public actions, including quarantines and forced treatment, may be justified; in the case of back pain, such actions would be wildly inappropriate.
A wide range of unhealthy behaviors could be framed in similar fashion. Smoking, skydiving, salting our food, motorcycling, freeway driving, and sleeping too little (to name a few) are all behaviors that increase our risk of illness or worse. If an increased risk of illness is all it takes to transform these behaviors into public health crises, then the government has a broad license to limit our freedom to do many potentially unhealthy things. Concentrating public health efforts on behaviors that hurt others, not just ourselves, lets us choose behaviors that make us happy while limiting the damage to others. If smoking causes secondhand damage, then it is a public health concern. If overeating brings only private costs, it is not.
Let us explore a television-inspired parable as a way of deciding whether the obesity epidemic is a public health crisis: Does Homer Simpson’s love of jelly doughnuts undermine the health and well-being of others in Springfield and beyond?

Pooled Health Insurance and Jelly Doughnuts
We can dismiss the idea that one person’s body weight decisions affect other people’s health. There is no mechanism, except perhaps indirectly and weakly, by which it might do so. (Does anyone really look to the overweight and underinhibited Homer Simpson as a role model for healthy living?) On the other hand, it is easy to think of mechanisms that might affect the well-being of others, the most important of which is pooled health insurance. Another is that obesity can reduce work productivity. It turns out, however, that the same sort of reasoning applies to both these mechanisms.
Here’s how pooled health insurance works: every member of the health insurance pool pays the same premium regardless of health status when signing up for the plan. In other words, Homer pays the same amount for health insurance coverage as his colleagues Carl and Lenny. This is true even though Homer is dangerously obese and likely to generate substantial medical costs in the coming year, while Carl and Lenny eat organic greens every day and have not sought medical care in years. By pooling together in the same insurance plan, Carl, Lenny, and all the other members subsidize Homer by the difference between Homer’s medical bills and the average medical bills of pool members.
It’s like going out to dinner with a large group of people, knowing beforehand that you are going to split the bill. Though we are loath to admit it, even sometimes to ourselves, dinners like that create a moral dilemma: do I order the lobster or the red snapper, which costs $20 less? If there are 20 people around the table, my lobster order will raise the bill by a dollar for everyone, including me, but I get to eat a meal that is $20 more expensive.
If the insurance pool is very large, Homer pays almost no part of the increased medical bills that are a consequence of his behavior. But the incentives created by pooling apply not just to Homer but to everyone else in the pool. For Carl, Lenny, and Homer alike, pooled health insurance reduces the total price of eating in unhealthy ways and avoiding the morning jog. If pool members were to respond to these incentives by eating more poorly and exercising less and if health insurance pooling were a common arrangement, then obesity truly would be a public health crisis. Relative to what would be socially optimal, pool members would weigh too much.
A note on Rugged Individualism
One important footnote bears on whether the obesity epidemic is a public health crisis. Up to now, I have been discussing body weight choices as if they are firmly under our control. As anyone who has tried a diet and failed can attest, this is naive. There are many influences on our diet and exercise choices that we can do little about. Though we are evolutionarily programmed to like sugar, fat, and salt, some of us seem constitutionally (dare I say genetically?) more resistant to the lure of chocolate cake than others.
Suppose that Homer overeats and fails to exercise because he can’t help himself, and that he would do the same whether he is in a health insurance pool or not. Surprisingly, Homer’s gluttony and sloth will cause no social loss.
Pooling still induces a transfer from Carl and Lenny to Homer, because Homer’s expected medical bills are higher than Carl’s and Lenny’s. Homer will be, say, a thousand dollars richer by dint of his participation in the pool, and the other pool members will be in aggregate a thousand dollars poorer. Because pool membership does not affect Homer’s behavior, however, there are no extra jelly doughnuts eaten or morning jogs forgone because of pooling. Pooling does induce a transfer, but it is a lossless transfer in which Homer’s gain exactly offsets the other pool members’ loss. It seems reasonable to require that any public health crisis generate some social loss. So, Carl and Lenny may not like being in the same pool as Homer, but that does not mean that the obesity epidemic is a public health crisis.
Ironically, this reasoning binds both rugged individualists who think that body weight is completely under individual control and determinists who think that obesity is socially determined, perhaps by Twinkie advertising or something else in our surroundings. The individualists tend to oppose muscular government action that would be appropriate if obesity were a public health crisis; yet if body weight is under individual control and influenced by incentives, there may be a social loss from pooled insurance and a public crisis. The determinists are often enthusiastic proponents of assertive public policy, yet their belief that body weight is not a choice implies that the obesity epidemic is not a public crisis, which undercuts the argument for the sorts of policies they favor.
AND NOW, THE MAIN COURSE: WHO PAYS?
Whether the obesity epidemic is a public health crisis thus turns on two empirical questions: How large is the subsidy induced by pooled insurance? And to what extent does the subsidy induce changes in body weight decisions? (That is, to what extent does health insurance make you fat?)
There is little evidence in the scholarly literature on the second question. In any case, the question is moot for employer-provided health insurance, which is the most common form in the United States. (The question is not moot in the case of government-provided health insurance, though.) With employer-provided health insurance, obese and nonobese workers are actually in separate risk pools. That is, obese workers pay more for health insurance than their thinner colleagues (see below). No matter what the answer to the second question, there is no social loss from pooling and no evidence of a public health crisis, at least via this mechanism.
Remember: even though employers nominally pay a substantial part of workers’ health insurance premiums, the workers themselves actually pay those premiums. How? Total compensation cannot exceed the value of the work done by the worker, at least in the long run. If it did, then the firm would lose money by hiring or retaining that worker. If total compensation is fixed, increases in health insurance premiums will be accompanied by reduced wages or smaller raises. Health insurance premiums thus are “passed through” to workers by means of wages.
Obese workers earn less per hour than their thinner colleagues—a finding that is surprisingly robust and does not appear to be explained by differences in education, age, or training. This obesity wage gap is greater for female workers, but it is also true for men. Most often, economists attribute the gap to discrimination against the obese. Occasionally, economists argue that in some jobs (think of supermodels), thinner workers are more productive than obese ones.
My colleague Kate Bundorf and I have developed evidence that favors a different explanation. We think an important reason for the obesity wage gap is that the costs of health insurance are passed through to obese workers. This would be consistent with the theory of wage pass-through, because expected medical expenditures and hence the value of health insurance are greater for obese workers than for thin workers.
In our research, we examined the wage path over a decade for a nationally representative cohort of 12,686 people ages 24 to 31 years old in 1989. For our study, we focused on full-time workers but excluded pregnant women. We separated the workers into two groups: one with health insurance provided by their employer and one without.
We first looked at the wage paths for the group with health insurance (see figure 1). As expected, given the discussion so far, obese workers earn less than thinner workers and the gap grows as the cohort ages and becomes more likely to use medical care. By 2000, obese workers were earning nearly $4.60 an hour less than thinner workers. This wage gap is at least as big as the expected difference in medical expenditures between obese and thin workers.
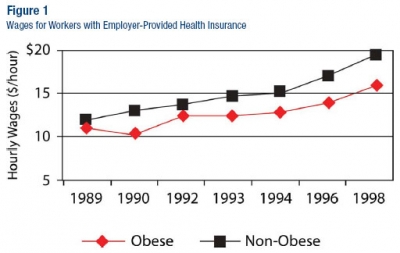
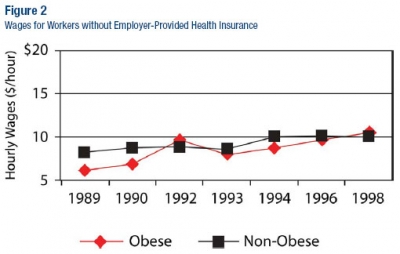
We then looked at wage paths for the group without health insurance (see figure 2). For this group, the obesity wage gap never develops—thin and obese workers earned about the same, on average, exactly what one would expect to find under the theory of wage pass-through.
Our evidence has important implications for pooling in health insurance between thin and obese workers. Because wages are lower for obese workers only at jobs where health insurance is provided, the obesity wage gap would seem to undo whatever nominal pooling there is of health insurance premiums. If there is no real pooling, Carl and Lenny do not pay for Homer’s body weight decisions and there is no public health crisis.
This reasoning does not extend to government-provided health insurance, which is also common in the United States but less so than private coverage. In 2004, there were 174.2 million Americans covered by employer health insurance, 39.7 million covered by Medicare (provided by the federal government to elderly and disabled people), and 37.5 million covered by Medicaid (provided by states to the poor). Under both Medicare and Medicaid, enrollees’ premiums do not depend on body weight and are always much lower than expected medical bills. In many cases, enrollees are not charged premiums at all. Unlike in employer-provided health insurance, there is no wage pass-through that can undo pooling between obese enrollees and taxpayers.
Studies on the size of the subsidy to obese enrollees induced by government health insurance are far from definitive, but it seems likely that the subsidy is substantial. We therefore return to an earlier question: does the subsidy induced by insurance change the body weight decisions of enrollees? If so, then at least under government-sponsored coverage, perhaps there is a public health problem after all.
The Social Harm from Obesity
Answering causal questions is notoriously difficult in the social sciences because controlled experiments are hard to run and “clean” natural experiments hard to find. So there is no definitive answer to whether enrollment in pooled insurance changes body weight decisions. However, my colleague Neeraj Sood and I have a tentative answer based on the extreme assumption that all Americans are in a single health insurance pool. This is like calculating the incentives to order the lobster when you are splitting the bill with every adult in the United States. Our model predicts (as far as possible) the body weight distribution of all adult Americans. Using this method, we found that the harm from distorted body weight decisions caused by this extreme pooling would be roughly $150 per adult per year. This means that on average, every adult American pays an extra $150 annually to subsidize the extra health care for obese people, roughly the price of one visit to the doctor.
While the focus of this article has been on investigating the social harm of obesity via pooled health insurance, similar reasoning can be brought to bear on other mechanisms. For instance, some economists have argued that obesity causes social harm by increasing the number of sick days from work, thus reducing workers’ productivity. Others have calculated that obese workers are more likely to file workers’ compensation claims than thinner employees. The key question, as always, is: do obese individuals pay for their lower productivity and higher injury rates or does someone else pay?
Though the question deserves a more careful look, I think it likely that obese workers themselves pay. It seems unlikely that employers would pay high wages to unproductive workers over any extended period. If that is so, then there is no social harm caused by this reduced productivity.
One might reason that there also is social harm from a reduction in a nation’s productivity. But such reasoning ignores the desires of the workers themselves. If each worker in a nation pays the full cost of her decisions leading to her lower productivity, then the nation is no poorer. In a sense, those workers are “buying” something they value—doughnuts, maybe—at the cost of lower productivity and lower wages.
Under the standard set out at the beginning of this essay, the obesity epidemic is no public health crisis. Most of the costs from poor diet and lack of exercise are paid by the obese themselves. This does not mean that the government should do nothing; for instance, it is probably appropriate to warn consumers about the dangers associated with some foods, such as those with high trans-fat content. Also, government should get out of the business of subsidizing foods (such as high-fructose corn syrup) through its agricultural policies.
Any government intervention should be scrutinized for unintended and harmful side effects. For instance, taxing burgers at fast-food restaurants may sound like a good idea, but doing so would hurt the poor. My colleagues Darius Lakdawalla and Tomas Philison have shown that raising the price of ground beef can increase anemia rates among poor children in the United States. That anemia rates and the price of ground beef rise together is not surprising because beef, often consumed at fast-food restaurants, is a primary source of iron for poor children. This is yet another warning against adopting policies appropriate for a public health crisis when no such crisis exists.
















