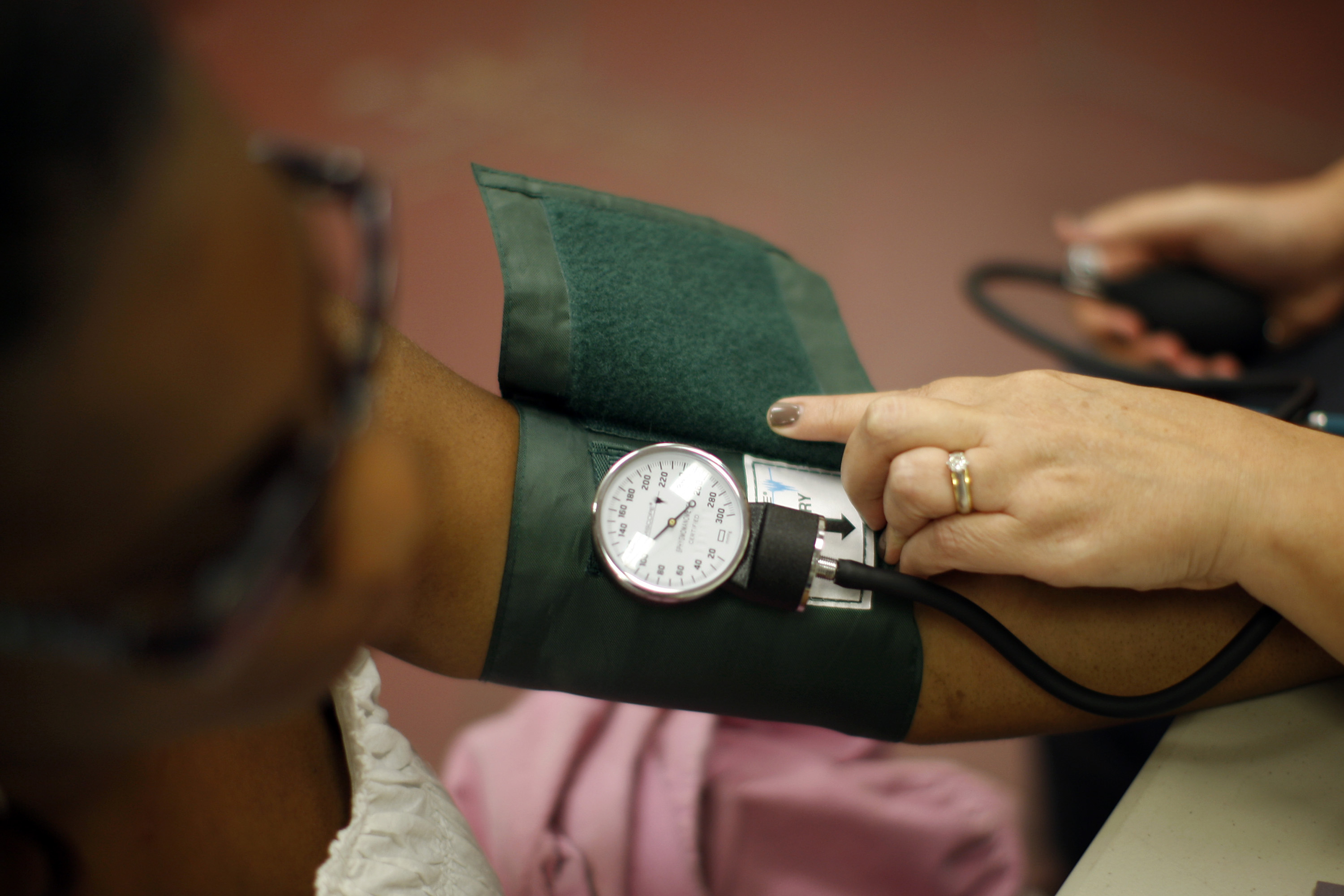
- Health Care
Editor’s note: A shorter version of this essay first appeared on CNN.com on September 25, 2017.
The Affordable Care Act is failing. Focused on shrinking the uninsured population, the law expanded government insurance programs and imposed considerable federal authority over U.S. health care via new mandates, regulations, and taxes. The harmful impacts of this ill-conceived approach should now be clear: Insurance premiums have skyrocketed even as deductibles rose; consumer choice on the state insurance marketplace has rapidly vanished; and for those with ACA coverage, doctor and hospital choices have narrowed dramatically. Meanwhile, consolidation across the health care sector has accelerated at a record pace, portending further harm to consumers, including higher costs in medical care.
Many Democrat and Republican leaders acknowledge these failures, but those proposing alternatives to the ACA are far from like-minded. Almost inexplicably, a truly radical change—single-payer health care—has found new support from the left, despite the documented failure of single-payer systems in other countries to provide timely, quality medical care—and despite similar problems in our own single-payer Veteran Affairs system. There is now decades’ worth of data chronicling the many shortcomings of single-payer health care, and how it falls far short of the superior access, broad freedom of choice, and exceptional quality of care found in American health care.
In those countries with the longest experience with single-payer government insurance, published data demonstrates that patients are held on massive waiting lists with unconscionable delays before receiving critical care. In the UK alone, more than 3.9 million patients are on the National Health System’s waiting lists; 362,600 patients waited longer than 18 weeks for hospital treatment in March 2017, an increase of almost 64,000 from the previous year; and 95,252 have been waiting more than six months for treatment—all after already receiving initial diagnosis and referral. As of late 2016, their average waiting time exceeded 100 days for hip or knee replacements, hernia, adenoid surgery, and tonsillectomies.
In Canada’s single-payer system, the 2016 median wait from general practitioner appointment to the specialist appointment was 9.4 weeks; when added to the median wait of 10.6 weeks from specialist to first treatment, the median wait after seeing a doctor to start treatment was 20 weeks, or about 4.5 months. For an appointment alone, a Canadian can expect to wait 12 weeks to see an ophthalmologist; over 32 weeks for a neurosurgeon; and over 15 for an orthopedist as they endure their bone and joint pain.
Ironically, U.S. media outrage was widespread when 2009 data showed that time-to-appointment for Americans averaged 20.5 days for five common specialties. But the reporters failed to note that those waits were mostly for check-ups of healthy patients, who are by definition the lowest medical priority. Even for simple physical exams and purely elective, routine appointments, U.S. wait times were shorter than for seriously ill patients in countries with nationalized, single-payer insurance.
For even the sickest patients, single-payer systems create shocking delays for medical care. Yes “everyone is insured,” but that’s a meaningless statement when people are dying while awaiting care in single-payer systems. That includes people referred by doctors for “urgent treatment” for already diagnosed cancer (almost 19 percent wait more than two months) and brain surgery (17 percent wait more than four months). In Canada’s single-payer system, the most recent data revealed a median wait for neurosurgery was a shocking 46.9 weeks, which is about 10 months. For those with heart disease, Canadians waited a median time of 8.4 weeks for their first treatment. And in Canada, if you needed life-changing orthopedic surgery, like hip or knee replacement, you would wait a startling 38 weeks—which is about how long it takes to create a full human life from fertilization to birth.
Americans enjoy the world’s earliest access to the newest prescription drugs, in stark contrast to patients in single-payer systems. Before the Affordable Care Act, the United States was the country where most new cancer drugs were first launched—and by a factor of at least four relative to Germany, Japan, Switzerland, France, Canada, Italy, and the UK—according to the Annals of Oncology in 2007. A 2011 Health Affairs study found that of 35 new cancer drugs submitted for approval between 2000 and 2011, the U.S. Food and Drug Administration (FDA) approved 32 while the European Medicines Agency (EMA) approved only 26. Median time to approval in the United States was about half that in Europe—and all 23 drugs approved by both were available to American patients first.
In Joshua Cohen’s 2006 study of patient access to 71 drugs, between 1999 and 2005 the UK government’s guidelines board NICE had been slower than the US to authorize 64 of these. Even in the most recent data, two-thirds of the novel drugs approved in 2015 (29 of 45, or 64%) were approved in the US before any other country. Indeed, Sweden finally privatized their pharmacies after decades of government ownership in response to severe problems with drug availability. And yet, only months ago, NHS England introduced a new “Budget Impact Test” to cap drug prices that is specifically designed to further restrict drug access, even though the delays will break their own NHS Constitution pledges to its citizens.
Problems abound with cancer screening tests, too. The facts show that single-payer systems cannot outperform the American system in something as scheduled and routine as cancer screening tests. Confirming numerous prior OECD studies, David Howard of Emory University reported in 2009 that prior to the ACA’s passage, the United States had superior screening rates compared to all 10 European countries with nationalized systems for all cancers. (Those countries included Austria, Denmark, France, Germany, Greece, Italy, the Netherlands, Spain, Sweden, and Switzerland.) Likewise, the single payer system of Canada fails to deliver screening tests for the most common cancers as broadly as the U.S. system does. And Americans are more likely to be screened younger for cancer than in Europe, when the expected benefit is greatest. Not surprisingly, when U.S. patients are diagnosed with cancer, their disease is at a less advanced stage than that of European patients. Data shows that single-payer systems have significantly worse outcomes from virtually all serious diseases, including cancer, heart disease, stroke, high blood pressure, and diabetes.
Contrary to the logic of those advocating for single-payer health care for America, and despite the intuitive attractiveness of the concept of a simpler system where the government explicitly “guarantees” medical care, single-payer insurance does not enable access to timely, quality medical care or good treatment outcomes. The truth is that the UK, Canada, Sweden, and other European countries have used waitlists as a means of rationing care for decades. And long waits for needed care are not simply inconvenient. Research has consistently shown that waiting for medical care has serious consequences, including pain and suffering, worse medical outcomes, and significant costs to individuals and the economy in foregone wages and productivity. Sometimes, the loss is far greater—too many patients in single-payer systems have died while waiting for critical care. In contrast, it is broadly acknowledged that “waiting lists are not a feature” of U.S. health care, in the words of Sharon Willcox of Health Policy Solutions in her Health Affairs study comparing strategies to measure and reduce this important failure of centralized health systems.
What has been the response to the public outcry about unacceptable waits for care in virtually all single-payer systems? First, a growing list of European governments—including Denmark, England, Finland, Ireland, Italy, the Netherlands, Norway, Spain, and Sweden—have issued dozens of decrees and “guarantees” of timely care with notably lax targets, even as those guarantees continue to be unmet. Second, many single-payer systems now funnel taxpayer money to private care to solve their systems’ inadequacies, just as we now do in our own VA system, and use taxpayer money for care in other countries, as codified in Section 3A of the NHS Constitution, as well. In one year alone, £901 million targeted for medical services by the UK government was used to buy care from private and other non-NHS providers, according to research by the Financial Times in March 2017.
Instead of working to expand the role of government or increasing subsidies, reforms should focus on making excellent medical care more broadly available and affordable. But there is a way to bring down the prices of medical care so that quality health care is made broadly available to all Americans. This can be accomplished without restricting its use or erecting obstacles to future innovation by creating conditions long proven to bring down prices while improving quality in all goods and services. Reducing the cost of medical care requires increasing the supply of medical care, stimulating competition among providers, and incentivizing empowered consumers to seek value for their money. Since almost 60 percent of all health expenditures is for elective outpatient care and only six percent is for emergencies, the impact of price-conscious consumers could be dramatic.
Detailed proposals based on such principles have been put forth, but leaders in Congress and the administration who support free market alternatives must do a better job of educating the public on the rationale and benefit of that approach. And make no mistake about it - America’s most vulnerable, the poor and the middle class, will undoubtedly suffer the most if the system turns to single payer health care, because only they will be unable to circumvent that system.
--
Scott W. Atlas is the David and Joan Traitel Senior Fellow at Stanford’s Hoover Institution and the author of Restoring Quality Health Care: A Six Point Plan for Comprehensive Reform at Lower Cost (Hoover Press, 2016).